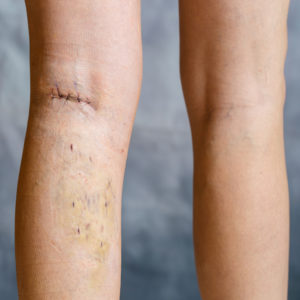
Chronic post surgical pain is defined as any pain that develops after a surgical procedure, lasts atleast 2 months in duration and other causes, including pre-exisiting pain, has been excluded. It is becomingly an increasingly recognised problem and upto 33% of patients report persistent or intermittent pain one year after common surgical procedures. A survey of 5000 patients attending outpatient pain clinics revealed that 22% of patients cited surgery as their main cause of chronic pain. This would still suggest significant underreporting since not all patients come into secondary care.
The common surgical procedures include inguinal hernia repair, breast surgery, orthopaedic and cardiothoracic surgery. The incidence of chronic pain is 12% for patietns undergoing hernia repair and is now the most common long term problem after such a surgery. Rates of CPSP are much higher after mastectomy with reconstruction (49%) compared to just mastectomy (31%). Upto 33% of Thoracic surgery patients are left with sever pain afterwards.
A number of putative risk factors have been identified which may contribute to development of CPSP. These include the presence of preoperative pain, age, intraoperative nerve handling/injury, surgical technique, psychological factors, severity of acute pain and perioperative anaesthetic management. As yet, there is no clear consensus on the mechanisms involved.
This increase in awareness of CPSP has led to a huge body of research looking into pre-emptive and preventative strategies. The challenge is to accurately identify at-risk patients and target suitable interventions. Many of the risk factors are difficult to influence or alter but two factors are clear.
1. Severity of acute postoperative pain influences CPSP. Effective treatment of acute pain after surgery can reduce the incidence of CPSP by preventing sensitisation of the central nervous system. This concept of ‘central sensitisation’ which can be blocked has led to a couple of strategies
a. Pre-emptive analgesia using drugs such as gabapentin or pregabalin along with opioids and NSAIDs/paracetamol administered preoperatively and continued postoperatively
b. Increased use of regional techniques such as epidurals/spinals and local anaesthetic blocks of peripheral nerves.
2. The second facor is having a surgical procedure. Inappropriate or unnecessary surgery needs to be prevented. Alternatives to surgery should be explored and patients must be made aware of risks so that a truly informed choice is made. Public education should be improved to both patients and their carers in order to help remove the belief that something must have gone wrong at the time of surgery.
Once CPSP has occurred, it is difficult to cure but there are a number of interventions that can be helpful in reducing pain. Initial management in primary care would include patient education, counselling and self management followed by the use of antineuropathic medication such as amitryptiline, gabapentin and pregabalin. Depending on the extent and severity of the pain and its effect on quality of life, pain specialists can employ a variety of interventions such as local infiltrations of steroids, diagnostic nerve blocks followed by pulsed radiofrequency in addition to managing patient expectation. When chosen appropriately, these techniques can provide long term relief.
